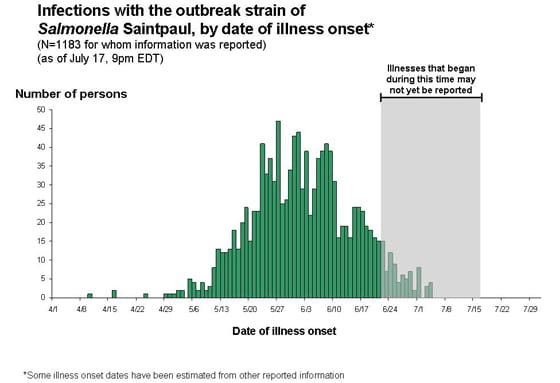
The latest CDC report on the ongoing Salmonella serotype Saintpaul suggests that we may indeed be nearing the end. Here is the epidemic curve as of 28 July:
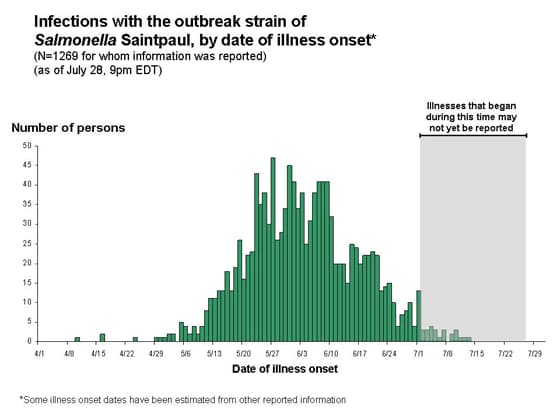
While there is certainly still the possibility of more cases appearing that have not yet been reported or another introduction (see previous post), the fact that the epidemic curve has continued to trail off in two successive weeks is good news.
The epidemiological evidence continues to implicate fresh jalapeño chiles grown in México. As of 28 July, 1307 cases have been reported since 1 April 2008. Nearly every state in the union has reported at least one case from this outbreak, as can be seen on this map:
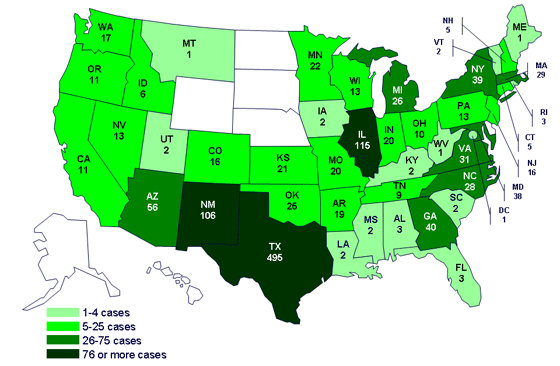
Again the most likely victims (at least to report illness) are 20-29 year-old adults while the least likely to report illness are 10-19 year-olds and those over 80. Once again, I suggest that this is consistent with a vehicle consumed along with alcoholic beverages. Salsa. Though contaminated jalapeños (or other produce) could, of course, make their way into other foods as well. The Saintpaul strain was relatively rare before this outbreak, leading CDC to suggest the following:
The previous rarity of this strain and the distribution of illnesses in all U.S. regions suggest that the implicated food is distributed throughout much of the country. Because many persons with Salmonella illness do not have a stool specimen tested, it is likely that many more illnesses have occurred than those reported.
Let's hope that this outbreak is really coming to an end. It would be nice if we could identify the source of the infection. Foodborne disease is an important public health concern that probably does not receive the attention it should. A 1999 paper by Mead and colleagues (admittedly now a bit long in the tooth) estimated that foodborne diseases cause approximately 76 million illnesses, 325,000 hospitalizations, and 5,000 deaths in the United States each year. It is not hard to imagine that in the 10 years since this study the foodborne disease burden has increased in the U.S. Time for another study, I'd say.